Mental Health Billing Toledo Ohio USA: A Complete Guide to Streamlining Practice Revenue
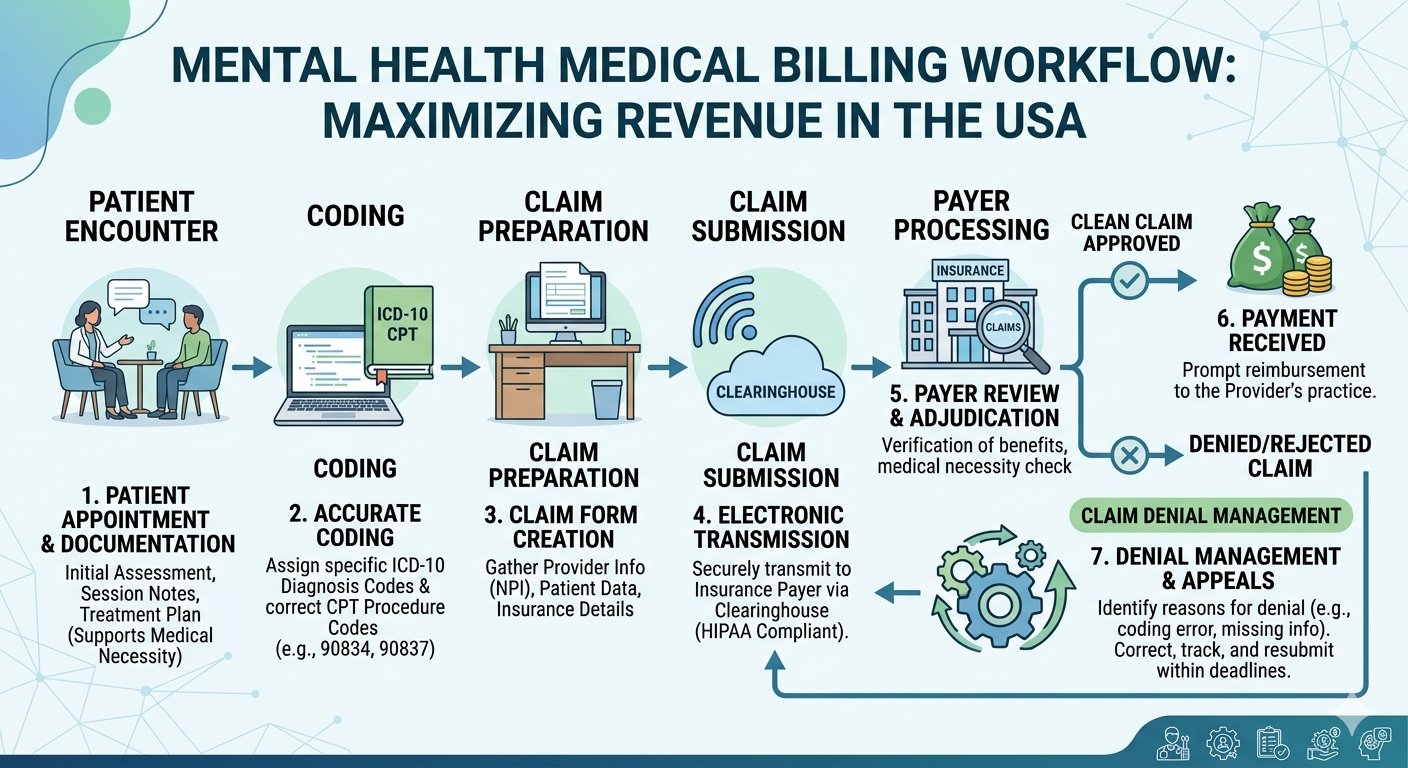
Mental health practices across Toledo are facing increasing administrative pressure while trying to deliver quality patient care. From insurance complexities to compliance requirements, billing has become one of the most critical yet time-consuming aspects of running a behavioral health practice. This is where mental health billing toledo ohio plays a vital role in ensuring financial stability and operational efficiency.
Whether you are a solo therapist, a psychiatric clinic, or a multi-specialty behavioral health provider, understanding how billing works and how to optimize it can directly impact your revenue and growth.
Why Mental Health Billing is Crucial for Toledo Practices
Mental health billing is more complex than general medical billing due to varying payer rules, therapy-specific codes, and strict documentation requirements. Providers in Toledo must deal with:
- Frequent claim denials due to incorrect coding
- Changing payer policies for behavioral health services
- Prior authorization requirements
- Compliance with state and federal regulations
- Time-consuming follow-ups on unpaid claims
Efficient mental health billing services ohio can help providers focus more on patient care while improving cash flow.
Key Components of Mental Health Billing
A successful billing process includes several interconnected steps:
Accurate Patient Information Collection
Collecting correct demographics and insurance details is the foundation of clean claims.
Insurance Verification
Verifying coverage ensures services are eligible for reimbursement and reduces claim rejections.
Medical Coding
Using correct CPT, ICD-10, and HCPCS codes is essential for therapy sessions, psychiatric evaluations, and medication management.
Claim Submission
Timely and error-free claim submission ensures faster processing.
Payment Posting and AR Follow-up
Tracking payments and following up on denied or underpaid claims improves revenue cycle efficiency.
Common Challenges in Mental Health Billing Toledo Ohio
Mental health providers in Toledo often face unique billing challenges:
- Complex coding for psychotherapy sessions
- Denials related to medical necessity
- Issues with telehealth billing compliance
- Coordination with multiple insurance providers
- Managing high accounts receivable
This is why many practices are turning toward outsourcing mental health billing ohio to specialized companies.
Benefits of Outsourcing Mental Health Billing
Outsourcing is becoming a preferred solution for practices looking to scale without administrative burden.
Improved Revenue Cycle
Professional billing teams reduce errors and increase claim acceptance rates.
Reduced Administrative Work
Providers can focus on patient care rather than paperwork.
Faster Reimbursements
Clean claims and proactive follow-ups lead to quicker payments.
Compliance Assurance
Billing companies stay updated with regulations and payer requirements.
Scalability
Outsourcing allows practices to grow without hiring in-house billing staff.
Many providers also explore outsourcing mental health billing services florida, outsourcing mental health billing texas, and outsourcing mental health billing virginia to understand nationwide best practices and benchmarks.
How to Choose the Right Mental Health Billing Partner
Selecting the right billing company is critical for long-term success. Consider the following:
- Experience in behavioral health billing
- Knowledge of local and national payer policies
- Transparent reporting and analytics
- Strong denial management process
- HIPAA compliance and data security
Some providers compare options like a mental health billing company georgia or a professional mental health billing company connecticut to evaluate expertise across different regions.
Statewide and Nationwide Billing Insights
While focusing on Toledo, it is beneficial to understand how billing practices differ across states. For instance:
- mental health billing services arizona focus heavily on telehealth compliance
- mental health billing services illinois emphasize payer-specific documentation
- mental health billing services north carolina often deal with Medicaid complexities
- mental health billing services texas require strict adherence to large payer networks
- mental health billing services virginia highlight credentialing challenges
Similarly, mental health billing services connecticut, mental health billing services rhode island, and mental health billing services tennessee showcase how regional regulations impact billing workflows.
Even smaller markets like mental health billing services cary and mental health billing agency delaware provide insights into localized payer expectations.
The Role of Technology in Mental Health Billing
Modern billing is driven by technology. Practices in Toledo are increasingly adopting:
- Electronic Health Records integration
- Automated claim scrubbing tools
- Real-time eligibility verification systems
- Advanced reporting dashboards
Technology reduces manual errors and enhances efficiency, especially when paired with a mental health billing services company georgia or mental health billing services company delaware that leverages advanced tools.
Compliance and Regulations in Ohio
Mental health providers must comply with:
- HIPAA regulations
- CMS guidelines
- Ohio Medicaid policies
- Telehealth billing rules
Failure to comply can lead to claim denials, audits, and financial penalties. This makes outsourcing mental health billing services connecticut or outsourcing mental health billing services delaware appealing for practices seeking compliance-driven workflows.
Credentialing and Its Impact on Billing
Credentialing is often overlooked but directly affects reimbursement. Without proper credentialing:
- Claims may be denied
- Payments may be delayed
- Providers may not be recognized by payers
A professional mental health billing company new hampshire or similar experienced providers often include credentialing support as part of their services.
Why Toledo Practices Are Moving Toward Outsourcing
Healthcare providers in Toledo are increasingly adopting outsourcing due to:
- Rising operational costs
- Staffing shortages
- Increasing billing complexity
- Need for faster reimbursements
Outsourcing mental health billing ohio allows practices to stay competitive while maintaining financial health.
Future Trends in Mental Health Billing
The future of mental health billing is evolving rapidly:
- Increased adoption of telehealth billing
- Value-based reimbursement models
- AI-driven claim analysis
- Enhanced data analytics for decision-making
Practices that adapt to these trends will have a competitive advantage in Toledo and beyond.
Conclusion
Mental health billing toledo ohio is more than just submitting claims; it is a strategic function that directly impacts the financial success of a practice. With increasing complexity in payer rules and compliance requirements, having a streamlined billing process is essential.
Partnering with experts or outsourcing billing services can significantly improve revenue, reduce administrative stress, and ensure compliance. As practices grow, integrating services like medical billing services, medical coding services, medical billing and coding services, revenue cycle management, and credentialing services becomes essential. Companies like 247 medical billing services help bridge the gap between patient care and financial performance, enabling providers to focus on what truly matters—delivering quality mental health care.
FAQs
What is mental health billing and how is it different from general billing?
Mental health billing involves specialized coding and documentation for behavioral health services, which differs from general medical billing due to therapy-specific requirements and payer rules.
Why is outsourcing mental health billing beneficial in Toledo Ohio?
Outsourcing reduces administrative burden, improves claim accuracy, and ensures faster reimbursements, helping practices maintain steady cash flow.
How do I choose the best mental health billing company?
Look for experience in behavioral health, strong denial management, compliance expertise, and transparent reporting.
What are the common reasons for claim denials in mental health billing?
Incorrect coding, lack of medical necessity, missing documentation, and insurance eligibility issues are common causes.
Is credentialing necessary for mental health billing?
Yes, credentialing ensures that providers are authorized by insurance companies, which is essential for receiving reimbursements.
Can small practices benefit from outsourcing billing services?
Absolutely. Even solo practitioners can improve efficiency and revenue by outsourcing billing tasks.
How long does it take to get paid for mental health claims?
Typically, it takes 2–4 weeks, but clean claims and efficient follow-ups can shorten this timeframe.
What role does technology play in billing?
Technology automates processes, reduces errors, and provides real-time insights into financial performance.





