Billing for Pain Management in USA: A Complete Guide to Streamlining Revenue and Reducing Claim Denials

Introduction
Billing in healthcare has never been simple, but when it comes to billing for pain management, the complexity increases significantly. Pain management practices deal with a wide range of procedures, frequent insurance verification challenges, and constantly changing payer guidelines. As a result, even small errors in documentation or coding can lead to claim denials and delayed reimbursements.
In the USA, where healthcare regulations and payer requirements differ across states and insurance providers, managing pain management medical billing efficiently is essential for financial stability. Clinics that fail to streamline their billing process often struggle with cash flow issues, compliance risks, and administrative overload.
This guide breaks down everything you need to know about medical billing for pain management, including challenges, best practices, outsourcing benefits, and how specialized services can improve revenue cycle performance.
Understanding Billing for Pain Management
Billing for pain management services involves coding, submitting, and tracking claims for procedures such as nerve blocks, epidural injections, physical therapy interventions, and medication management.
Unlike general practice billing, pain management requires deep knowledge of procedural coding and documentation accuracy because:
- Multiple procedures may occur in a single visit
- Modifier usage is frequent and critical
- Prior authorizations are often mandatory
- Payer rules vary widely for interventional procedures
A strong pain management billing service ensures that each procedure is properly documented and reimbursed without delays or rejections.
Key Challenges in Pain Management Medical Billing
Pain management clinics face several billing-related challenges that directly impact revenue.
1. Complex Coding Requirements
Pain management procedures rely heavily on CPT and ICD-10 codes. Even minor mistakes in coding can lead to claim denials or underpayments.
2. Frequent Insurance Denials
Insurance companies often reject claims due to missing documentation, incorrect modifiers, or lack of prior authorization.
3. Changing Payer Policies
Payers regularly update reimbursement rules, making it difficult for in-house teams to stay compliant.
4. High Administrative Burden
Clinics often struggle to balance patient care with administrative tasks like billing and coding.
5. Delayed Payments
Improper claim submission results in longer reimbursement cycles, affecting cash flow.
These challenges highlight why many practices consider outsourcing pain management billing services to specialized providers.
Core Elements of Pain Management Medical Billing
To achieve accuracy and efficiency, several components must work together in the billing cycle.
Accurate Medical Coding Services
Proper coding ensures that every procedure is correctly classified. Professional medical coding services help reduce errors and ensure compliance with payer guidelines.
Efficient Claim Submission
Timely submission of claims ensures faster reimbursements and reduces revenue leakage.
Documentation Management
Detailed clinical documentation supports every billed procedure and minimizes audit risks.
Denial Management
A strong denial management system helps identify patterns and reduce future claim rejections.
Revenue Tracking
Monitoring payments and outstanding claims ensures a steady revenue flow.
Together, these processes form the foundation of effective pain management medical billing services.
Why Pain Management Billing Requires Specialization
Unlike general medical billing, medical billing pain management requires expertise in interventional procedures, anesthesia coding, and chronic care billing models.
Specialized pain management billing companies understand:
- Epidural steroid injection billing rules
- Facet joint procedures and coding guidelines
- Nerve block documentation requirements
- Compliance with CMS regulations
This specialization helps clinics maximize reimbursements while minimizing compliance risks.
Benefits of Outsourcing Pain Management Billing
Many healthcare providers now prefer to outsource pain management billing instead of handling it in-house.
1. Improved Revenue Cycle Efficiency
Professional billing teams optimize every stage of the revenue cycle, from patient intake to final payment.
2. Reduced Claim Denials
Experts ensure accurate coding and documentation, reducing rejection rates significantly.
3. Cost Savings
Outsourcing eliminates the need for hiring, training, and maintaining an in-house billing department.
4. Faster Payments
Streamlined workflows lead to quicker claim processing and reimbursements.
5. Focus on Patient Care
Physicians can focus more on treatment instead of administrative tasks.
Many clinics choose outsourcing pain management billing services to improve operational efficiency and financial performance.
Role of Revenue Cycle Management in Pain Management Billing
A strong revenue cycle management services framework is essential for pain management practices. It ensures that every stage of billing—from patient registration to final payment—is optimized.
Key functions include:
- Insurance eligibility verification
- Charge capture and coding accuracy
- Claims submission and tracking
- Payment posting and reconciliation
- Denial and appeal management
When implemented correctly, RCM significantly improves revenue flow and reduces administrative stress.
Importance of Credentialing in Pain Management Practices
Before providers can bill insurance companies, they must be properly enrolled. This is where credentialing services play a crucial role.
Credentialing ensures:
- Provider eligibility with insurance networks
- Compliance with payer requirements
- Faster onboarding for new physicians
- Reduced claim rejections due to enrollment issues
Without proper credentialing, even accurate billing cannot guarantee reimbursement.
Best Practices for Pain Management Billing Success
To improve efficiency and reduce revenue loss, pain management clinics should follow these best practices:
- Maintain accurate and updated patient records
- Verify insurance eligibility before every visit
- Use correct CPT and ICD-10 codes
- Apply modifiers appropriately
- Train staff regularly on payer updates
- Conduct periodic billing audits
These practices significantly improve the effectiveness of pain management billing and coding services.
Choosing the Right Pain Management Billing Company
Selecting the right pain management medical billing company can make a major difference in financial performance.
When evaluating providers, consider:
- Industry experience in pain management billing
- Technology and automation capabilities
- Denial management success rate
- Transparency in reporting
- Compliance with HIPAA regulations
A reliable pain management billing company acts as a strategic partner rather than just a service provider.
Future of Pain Management Billing in the USA
The future of billing for pain management in the USA is evolving rapidly due to technology and regulatory changes.
Key trends include:
- Increased use of AI in medical coding
- Automation of revenue cycle processes
- Value-based care reimbursement models
- Enhanced data analytics for billing insights
- Stronger compliance enforcement
Clinics that adapt to these changes early will gain a competitive advantage in revenue optimization.
Why Outsourcing is Becoming the Standard
More healthcare providers are moving toward outsourcing pain management billing services because it ensures accuracy, compliance, and financial stability.
With rising administrative burdens and stricter payer rules, outsourcing has become a strategic decision rather than just a cost-saving measure.
Conclusion
Efficient billing for pain management is essential for the financial success of any pain management practice in the USA. From accurate coding to denial management and compliance, every step in the billing cycle plays a critical role in revenue generation.
Partnering with a trusted expert like 247 Medical Billing Services can help clinics simplify operations and improve financial outcomes. Their expertise in medical billing services, medical coding services, medical billing and coding services, revenue cycle management services, and credentialing services ensures end-to-end support for healthcare providers.
By leveraging specialized support and modern billing strategies, pain management practices can reduce claim denials, improve cash flow, and focus more on delivering quality patient care.
Frequently Asked Questions (FAQs)
1. What is billing for pain management?
Billing for pain management refers to the process of coding, submitting, and managing insurance claims for pain-related medical procedures such as injections, nerve blocks, and therapy treatments.
2. Why is pain management medical billing so complex?
It involves multiple procedures, strict documentation requirements, frequent use of modifiers, and constantly changing payer rules, making it more complex than general medical billing.
3. Should clinics outsource pain management billing services?
Yes, outsourcing helps reduce errors, improve reimbursement speed, and allow providers to focus on patient care instead of administrative work.
4. What are the benefits of revenue cycle management services?
They streamline billing operations, reduce claim denials, improve cash flow, and ensure end-to-end financial efficiency.
5. How do credentialing services impact billing?
Credentialing ensures providers are properly enrolled with insurance companies, which is necessary for claim approvals and timely payments.
6. How do pain management billing companies improve revenue?
They use expert coding, denial management strategies, and compliance checks to maximize reimbursements and reduce revenue leakage.
Kategoriler
Read More
Treatment will be probably the most beneficial solutions in modern skin care and wonder routines. Most people work with ointment each day to keep their skin gentle even sunbed cream plus healthy. Treatment is not only well-liked by girls but trusted by way of men plus children. Various kinds of ointment are available for different skin requirements rendering it a crucial part of personal...

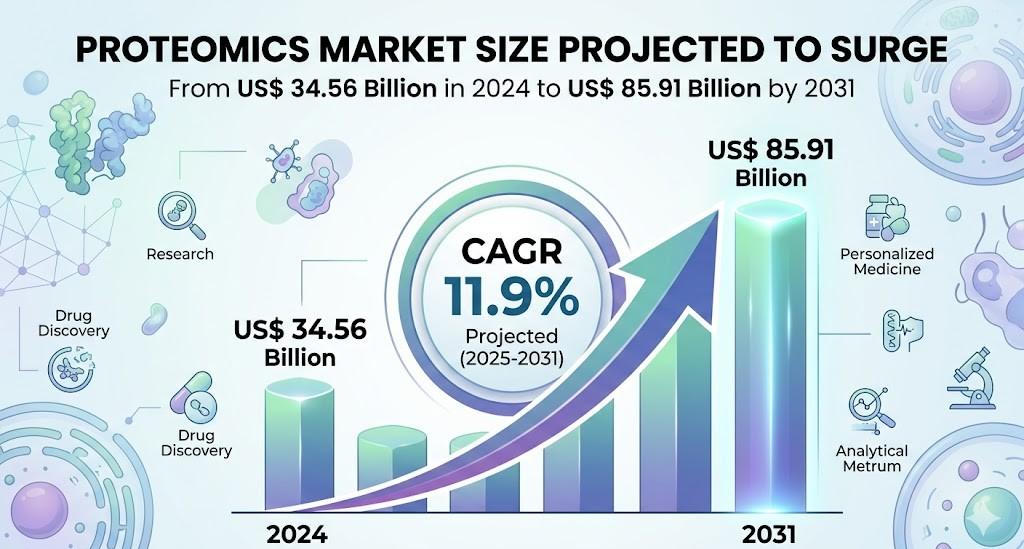
The global proteomics industry is witnessing strong structural transformation driven by rising demand for advanced protein analysis in biomedical research, drug development, and clinical diagnostics. Increasing focus on precision medicine and biomarker discovery is accelerating the adoption of proteomics technologies across pharmaceutical companies, research institutes, and healthcare...
InsuLeaf is a daily supplement designed for adults in the USA who want support in maintaining healthy blood sugar levels as part of a balanced lifestyle. Many individuals experience energy fluctuations, cravings, and inconsistent focus throughout the day. InsuLeaf works with the body’s natural processes to help maintain blood sugar levels already within a normal range, promoting...

A new growth forecast report titled Aminophylline Market Share, Size, Trends, Industry Analysis Report, By Application (Asthma, Chronic Obstructive Pulmonary Disease (COPD), Infant Apnea, Others); By Route of Administration; By Distribution Channel; By Region; Segment Forecast, 2024- 2032 introduced by Polaris Market Research represents conclusive data on the overall market. It majorly targets...

Something’s changed over the last few years. Not loudly, not in a “big announcement” kind of way. But quietly, companies started realizing the cloud alone isn’t enough anymore. Data moves too fast. Users expect instant responses. Waiting for a server sitting miles away? That delay adds up. That’s where Edge AI Solutions with AWS starts to make sense. It’s not...


