Varicocele: Causes, Symptoms, Diagnosis, Treatment, and Prevention
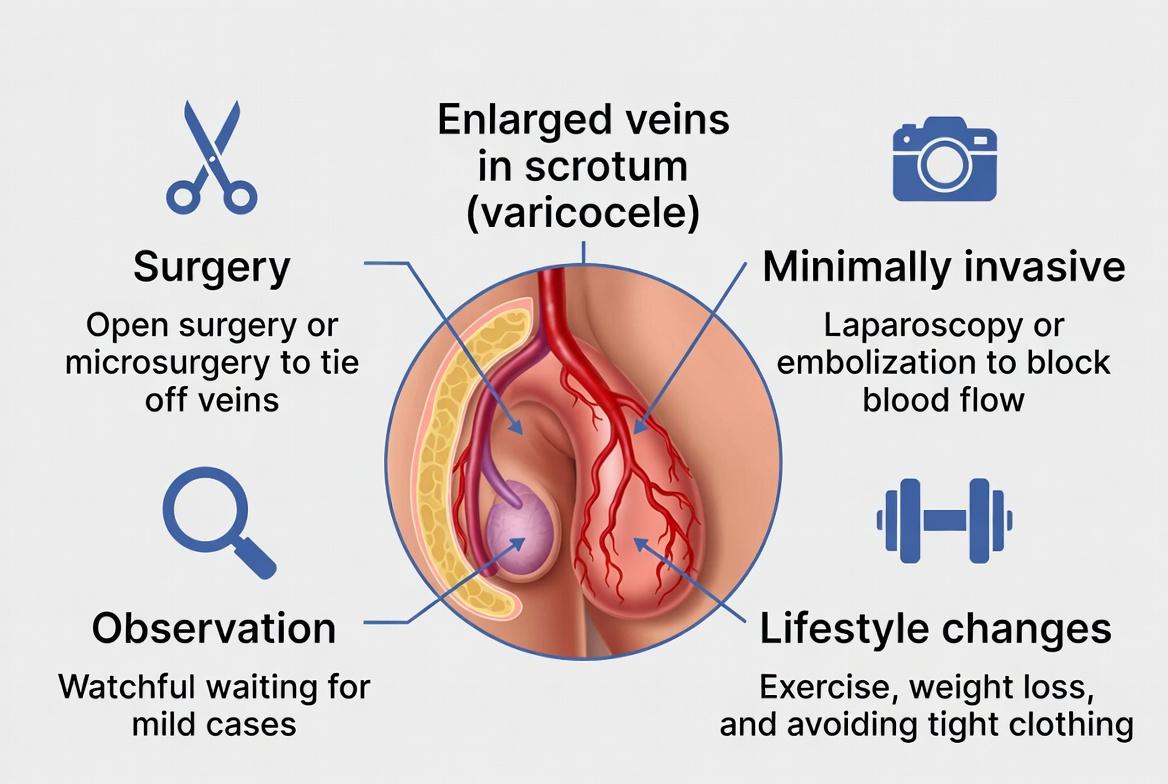
Varicocele is one of the most common disorders affecting the male reproductive system. It is characterized by the enlargement and twisting of veins inside the scrotum, specifically within the pampiniform plexus, a network of veins responsible for draining blood from the testicles. The condition is often compared to varicose veins in the legs because both involve abnormal swelling of veins due to faulty blood flow.
Although varicocele is not usually life-threatening, it can significantly affect male reproductive health. It is recognized as one of the leading reversible causes of male infertility worldwide. Many men with varicocele experience no symptoms, while others may suffer from scrotal pain, heaviness, reduced testosterone levels, shrinking of the testicles, and fertility issues.
Varicocele commonly develops during puberty and may gradually worsen over time if left untreated. Modern medical treatments, including minimally invasive procedures and microsurgical techniques, have made varicocele highly treatable with excellent success rates.
This comprehensive article provides detailed information about varicocele, including its causes, risk factors, symptoms, diagnosis, treatment options, complications, prevention strategies, and long-term outcomes.
Understanding Varicocele
A varicocele occurs when the veins within the spermatic cord become enlarged due to improper blood flow. The spermatic cord contains arteries, veins, nerves, and the vas deferens, which transports sperm from the testicles.
Under normal conditions, blood flows smoothly from the testicles back toward the heart through one-way valves located inside the veins. When these valves fail to function properly, blood begins to flow backward and accumulates in the veins. This causes the veins to enlarge and become twisted.
Varicocele most frequently affects the left side of the scrotum because the anatomy of the left testicular vein creates higher pressure compared to the right side. However, bilateral varicocele involving both sides can also occur.
Anatomy of the Male Reproductive Veins
Understanding the anatomy helps explain why varicocele develops.
The pampiniform plexus is a collection of interconnected veins surrounding the testicular artery. These veins serve an important function in temperature regulation. Sperm production requires temperatures slightly lower than normal body temperature. The pampiniform plexus cools arterial blood before it reaches the testicles.
When varicocele develops:
- Blood stagnates in the veins
- Heat accumulates around the testes
- Oxygen delivery becomes impaired
- Toxins and waste products build up
This altered environment negatively affects sperm production and testicular function.
Causes of Varicocele
The exact cause of varicocele is not always known, but several contributing factors have been identified.
1. Defective Vein Valves
The primary cause is the malfunction of one-way valves inside the veins. Normally, these valves ensure upward blood flow toward the heart. If they weaken or fail, blood flows backward and pools in the scrotal veins.
2. Increased Venous Pressure
Pressure inside abdominal veins may interfere with blood drainage from the testicles. This increased pressure stretches the veins and leads to enlargement.
3. Left-Sided Vein Anatomy
The left testicular vein drains into the left renal vein at a 90-degree angle, which creates higher venous pressure. In contrast, the right testicular vein drains directly into the inferior vena cava, allowing smoother blood flow.
This anatomical difference explains why approximately 80–90% of varicoceles occur on the left side.
4. Genetic Factors
Some men inherit weak vein walls or defective valves, increasing their susceptibility.
5. Rapid Growth During Puberty
Increased blood supply to reproductive organs during puberty may contribute to the development of varicocele.
Types and Grading of Varicocele
Doctors classify varicoceles according to size and severity.
Grade 0 (Subclinical Varicocele)
- Not visible or palpable
- Detected only through ultrasound
Grade 1 (Small)
- Felt only during straining or coughing
- Not visible externally
Grade 2 (Moderate)
- Easily felt during physical examination
- Not visible
Grade 3 (Large)
- Clearly visible through the scrotal skin
- Often resembles a “bag of worms”
Symptoms of Varicocele
Many men remain asymptomatic for years. Others may experience symptoms that vary in severity.
1. Scrotal Pain and Discomfort
Pain is one of the most common complaints.
Characteristics include:
- Dull aching sensation
- Heaviness in the scrotum
- Worsening pain after standing
- Increased discomfort after exercise
- Relief when lying down
2. Enlarged or Twisted Veins
Visible enlarged veins may appear above the affected testicle.
3. Testicular Shrinkage (Atrophy)
The affected testicle may become smaller because impaired circulation damages testicular tissue.
4. Fertility Problems
Varicocele can reduce sperm quality and production.
5. Scrotal Swelling
Large varicoceles may cause noticeable swelling or asymmetry.
How Varicocele Affects Fertility
Varicocele is strongly associated with male infertility. It affects sperm production through multiple mechanisms.
Increased Scrotal Temperature
Healthy sperm production requires cooler temperatures than the rest of the body. Enlarged veins interfere with the cooling mechanism, increasing testicular temperature and damaging sperm cells.
Oxidative Stress
Poor blood circulation increases harmful molecules called reactive oxygen species (ROS). These molecules damage sperm DNA and reduce sperm quality.
Reduced Oxygen Supply
Blood pooling decreases oxygen delivery to the testes, impairing sperm production.
Hormonal Imbalance
Varicocele may damage Leydig cells, which produce testosterone.
DNA Fragmentation
Sperm DNA may become fragmented, reducing fertility potential and increasing miscarriage risk.
Effects of Varicocele on Sperm Parameters
Men with varicocele may develop:
- Low sperm count
- Poor sperm motility
- Abnormal sperm shape
- Reduced semen volume
- Poor sperm concentration
- Increased sperm DNA damage
Risk Factors for Varicocele
Several factors may increase the likelihood of developing varicocele.
Age
Varicocele commonly develops between ages 15 and 25.
Family History
A family history of venous disorders may increase risk.
Heavy Physical Activity
Frequent heavy lifting increases abdominal pressure.
Obesity
Excess weight may impair blood circulation.
Chronic Constipation
Straining increases pressure in abdominal veins.
Prolonged Standing
Standing for long periods may worsen venous pooling.
Diagnosis of Varicocele
Early diagnosis is important for preserving fertility and preventing complications.
Medical History
Doctors ask about:
- Pain symptoms
- Fertility concerns
- Testicular changes
- Duration of symptoms
Physical Examination
The examination is usually performed while standing.
The physician may:
- Palpate enlarged veins
- Ask the patient to strain or cough
- Assess testicular size
Large varicoceles often feel like a “bag of worms.”
Ultrasound Imaging
Scrotal ultrasound is the gold standard diagnostic tool.
It helps:
- Confirm enlarged veins
- Measure blood flow reversal
- Detect subclinical varicocele
- Exclude tumors or other conditions
Doppler ultrasound is especially useful for evaluating blood circulation.
Semen Analysis
Men with fertility problems undergo semen testing to evaluate:
- Sperm count
- Motility
- Morphology
- Semen volume
Abnormal results may indicate fertility impairment.
Hormone Testing
Blood tests may measure:
- Testosterone
- Follicle-stimulating hormone (FSH)
- Luteinizing hormone (LH)
Complications of Varicocele
Untreated varicocele may lead to serious complications.
1. Male Infertility
The most significant complication.
2. Testicular Atrophy
Long-term damage causes shrinkage of the affected testicle.
3. Chronic Pain
Persistent pain may interfere with daily life.
4. Low Testosterone Levels
Hormonal production may decline over time.
5. Psychological Stress
Infertility and chronic discomfort may affect mental health and relationships.
Treatment of Varicocele
Treatment depends on:
- Severity of symptoms
- Fertility goals
- Age
- Semen abnormalities
- Testicular growth issues
Conservative Management
Mild cases without fertility problems may only require observation.
Lifestyle Modifications
Patients are advised to:
- Avoid heavy lifting
- Reduce prolonged standing
- Wear supportive underwear
- Maintain healthy weight
Pain Relief
Over-the-counter medications such as ibuprofen may reduce discomfort.
Surgical Treatment Options
Surgery is recommended for:
- Persistent pain
- Infertility
- Testicular shrinkage
- Abnormal semen analysis
Varicocelectomy
Varicocelectomy is the surgical correction of varicocele.
The surgeon ties or seals enlarged veins to redirect blood through healthy vessels.
Types of Varicocelectomy
1. Microsurgical Varicocelectomy
Considered the gold standard.
Advantages:
- Highest success rates
- Lowest recurrence risk
- Minimal complications
- Faster recovery
A surgical microscope allows precise identification of veins while preserving arteries and lymphatics.
2. Open Surgery
Traditional technique using a small groin incision.
3. Laparoscopic Surgery
Performed using a camera and small instruments inserted through the abdomen.
Benefits include:
- Smaller incisions
- Reduced pain
- Short hospital stay
Varicocele Embolization
A minimally invasive radiological procedure.
During embolization:
- A catheter is inserted into a vein
- Tiny coils or chemicals block abnormal veins
- Blood reroutes naturally
Benefits:
- No surgical incision
- Quick recovery
- Minimal pain
However, recurrence rates may be slightly higher compared to microsurgery.
Recovery After Varicocele Treatment
Recovery varies depending on the procedure.
After Surgery
Patients may experience:
- Mild swelling
- Bruising
- Temporary discomfort
Most men return to work within one week.
Heavy exercise should be avoided for several weeks.
After Embolization
Recovery is usually faster.
Most patients resume normal activities within 24–48 hours.
Improvement in Fertility After Treatment
Many men experience significant improvements after treatment.
Possible benefits include:
- Increased sperm count
- Better sperm motility
- Improved sperm morphology
- Higher testosterone levels
- Increased pregnancy rates
Improvement may take 3–6 months because sperm production cycles require time.
Recurrence of Varicocele
Varicocele can recur after treatment.
Risk factors include:
- Incomplete closure of veins
- Poor surgical technique
- Complex vein anatomy
Microsurgical techniques have the lowest recurrence rates.
Varicocele in Adolescents
Adolescents with varicocele require careful monitoring.
Doctors evaluate:
- Testicular growth
- Pain symptoms
- Fertility risk
Surgery may be recommended if one testicle becomes significantly smaller.
Varicocele and Testosterone
Varicocele may impair testosterone production by damaging Leydig cells inside the testes.
Low testosterone symptoms may include:
- Fatigue
- Reduced libido
- Erectile dysfunction
- Muscle loss
- Mood changes
Treatment may improve hormone levels in many men.
Natural and Lifestyle Support for Varicocele
Although lifestyle changes cannot cure varicocele, they may reduce symptoms and support fertility.
Healthy Diet
Consume foods rich in:
- Antioxidants
- Vitamin C
- Zinc
- Selenium
- Omega-3 fatty acids
Exercise Regularly
Moderate exercise improves circulation.
Avoid Excessive Heat Exposure
Limit:
- Hot baths
- Saunas
- Tight clothing
Stop Smoking
Smoking damages sperm and blood vessels.
Limit Alcohol
Excessive alcohol may impair fertility.
Prevention of Varicocele
Complete prevention may not always be possible because anatomy plays a major role. However, healthy habits may reduce progression.
Prevention Tips
- Avoid chronic straining
- Maintain healthy body weight
- Stay physically active
- Wear supportive underwear
- Avoid prolonged standing
- Manage constipation early
When to Consult a Doctor
Seek medical attention if you notice:
- Scrotal pain
- Swollen veins
- Fertility difficulties
- Testicular shrinkage
- Changes in scrotal appearance
Early treatment improves outcomes and protects fertility.
Frequently Asked Questions (FAQs)
Is varicocele dangerous?
Varicocele is usually not life-threatening but may affect fertility and testosterone production.
Can varicocele cause erectile dysfunction?
Indirectly, low testosterone associated with varicocele may contribute to erectile issues.
Does every varicocele need surgery?
No. Many mild cases only require observation.
Can varicocele return after surgery?
Yes, although recurrence is less common with microsurgical repair.
Can varicocele affect both testicles?
Yes, bilateral varicoceles can occur.
How common is varicocele?
It affects approximately 15% of men worldwide.
Conclusion
Varicocele is a common condition involving enlargement of scrotal veins that can significantly affect male reproductive health. Although many men remain symptom-free, others may experience chronic pain, testicular shrinkage, hormonal imbalance, and infertility.
The condition is one of the most common reversible causes of male infertility, making early diagnosis and proper management extremely important. Advances in microsurgery and minimally invasive procedures have greatly improved treatment outcomes and fertility success rates.
Men experiencing scrotal discomfort, visible swollen veins, or fertility issues should seek medical evaluation promptly. Timely treatment can preserve testicular function, improve fertility potential, restore hormone balance, and enhance overall quality of life.
Catégories
Lire la suite
Backyards in Glen Ridge are changing in a big way. They are no longer just grass and a few plants. Today, families want outdoor spaces where they can sit, cook, play, and relax. The newest ideas in Landscape Design in Glen Ridge, NJ, focus on comfort, smart layouts, and easy care. This means adding outdoor sofas, fire pits, and simple gardens that look good all year. This guide explains the top...

Eye strain, dryness, redness, and fatigue have become common problems in today’s screen-focused world. Prolonged exposure to digital devices, artificial lighting, and environmental stress can negatively affect vision and eye comfort. EyeBoost is a natural eye care supplement designed to support long-term eye health, enhance visual clarity, and reduce discomfort. With its blend...

The global Biometric Card Readers market has expanded from $1.2 billion in 2016 to $1.9 billion in 2021, reflecting a CAGR of 9.5%. Rising demand for secure access control, government regulations, and corporate security initiatives are driving adoption. The market is projected to reach $2.7 billion by 2027, at a CAGR of 12.5% between 2021 and 2027, fueled by advanced fingerprint, iris, and...

A practical Generative AI in Oil and Gas Market Solution is typically designed as a secure copilot that augments engineers, operators, and maintenance staff. The solution combines a hosted model (often private), retrieval over curated internal knowledge, and integrations with operational systems. Common capabilities include summarizing drilling and production reports, drafting work...

Legal Free Streaming Platforms If you're on the hunt for legal and safe options to stream movies and TV shows without spending a dime, there are numerous platforms available globally. These sites offer a wide array of content, from current hits to classic favorites, ensuring you can find entertainment suited to your taste without risking malware or copyright issues. Many free streaming...


