Mental Health Billing Services in USA: Complete Guide for Providers
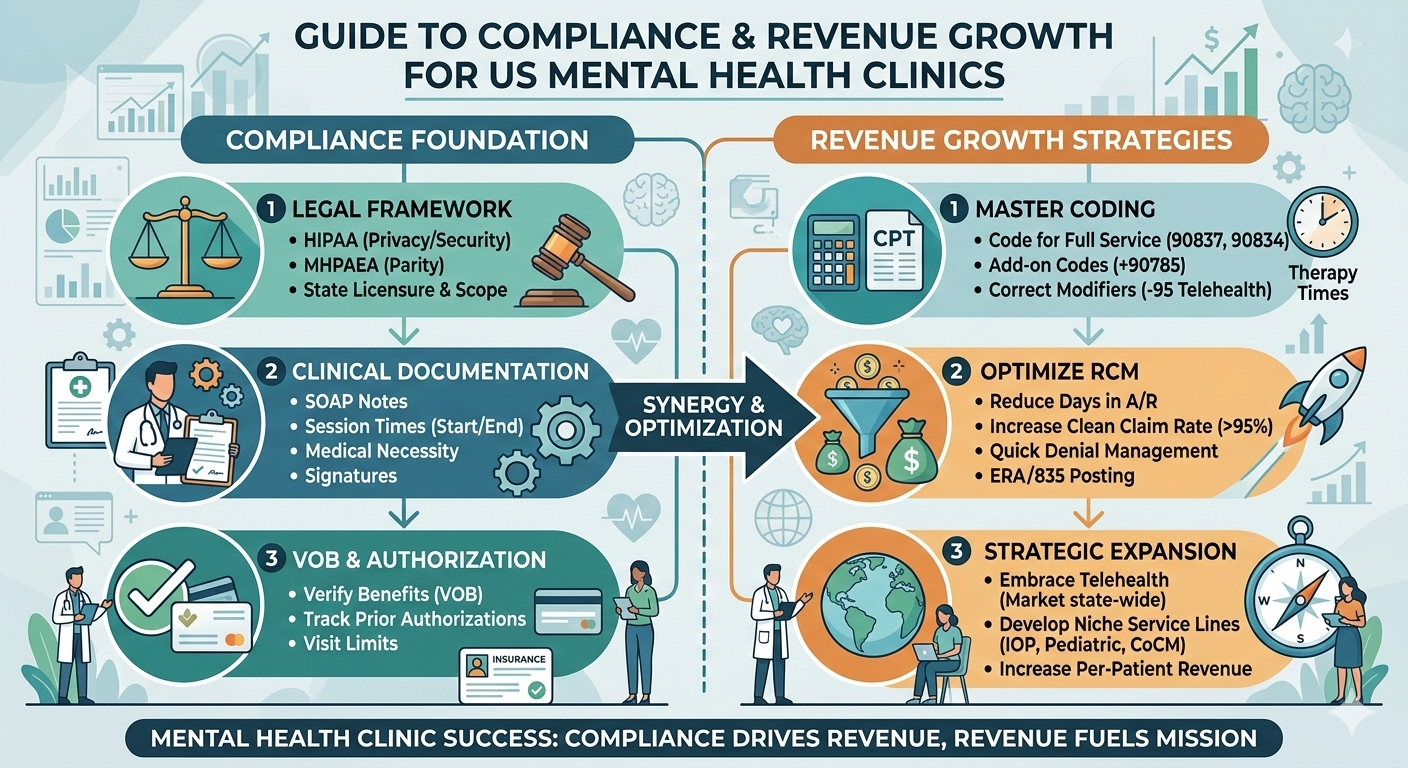
Mental health practices across the United States are experiencing steady growth. With rising awareness, expanded insurance coverage, and telehealth adoption, providers are seeing more patients than ever before. But along with this growth comes a complex financial responsibility: managing accurate, compliant, and timely billing.
Mental health billing services have become essential for practices that want to reduce denials, improve cash flow, and stay compliant with payer regulations.
In this guide, you will learn:
-
Why billing for mental health providers is more complex than general medical billing
-
How outsourcing mental health billing improves collections
-
What to expect from a professional mental health billing services company
-
Key compliance areas including Medicare and credentialing
-
How to choose the best mental health billing company in the USA
Understanding the Complexity of Mental Health Billing
Billing for mental health is not as straightforward as submitting a standard office visit claim. Therapy sessions, psychiatric evaluations, group therapy, telehealth visits, and medication management all require precise coding and documentation.
Coding and billing for mental health services involves:
-
Accurate use of CPT and HCPCS codes
-
Proper time-based documentation
-
Modifiers for telehealth and place of service
-
Coordination of benefits
-
Authorization tracking
Unlike other specialties, behavioral and mental health billing services often deal with session duration requirements, frequency limitations, and payer-specific psychotherapy rules. Even a minor documentation gap can result in claim rejection.
Medical billing for mental health must also align with HIPAA standards, payer contracts, and federal regulations, particularly when billing Medicare for mental health services.
Why Mental Health Practices Struggle With In-House Billing
Many providers initially attempt to manage billing internally. However, as patient volume increases, administrative pressure builds.
Common challenges include:
-
High denial rates due to coding errors
-
Delays in prior authorizations
-
Incomplete documentation
-
Frequent payer policy changes
-
Credentialing delays
Billing mental health claims requires specialized knowledge. General billing companies for mental health may lack behavioral health expertise, leading to repeated errors.
When providers spend hours correcting claims, following up with insurance, and reconciling payments, clinical care often suffers.
The Role of a Mental Health Billing Services Company
A professional mental health billing company focuses exclusively on behavioral healthcare reimbursement. Their teams understand therapy billing rules, psychiatric coding guidelines, and payer nuances.
A mental health billing services company typically manages:
-
Insurance verification and eligibility checks
-
Prior authorizations
-
Claim submission and tracking
-
Denial management and appeals
-
Payment posting
-
Accounts receivable follow-up
-
Reporting and revenue analysis
By handling the entire revenue cycle, mental health billing specialist companies allow providers to focus on patient care rather than administrative tasks.
Benefits of Outsourcing Mental Health Billing
Outsourcing mental health billing and coding can significantly improve practice performance. Here’s how:
Improved Cash Flow
Dedicated billing teams reduce claim rejections and speed up reimbursements.
Reduced Administrative Burden
Staff can focus on scheduling, patient communication, and front-desk efficiency instead of insurance calls.
Lower Operational Costs
Hiring and training in-house billing staff can be expensive. Outsourced billing for mental health eliminates payroll overhead.
Compliance Protection
Mental health billing solutions ensure compliance with federal and state regulations, including Medicare guidelines.
Scalability
As your practice grows, billing services for mental health clinics can scale without requiring new hires.
Many providers searching for the best outsource mental health billing and coding services are primarily looking for reliability and transparency in reporting.
Key Services Included in Mental Health Billing Solutions
A comprehensive mental health medical billing service should go beyond basic claim submission.
Insurance Credentialing
Mental health billing and credentialing services help providers enroll with payers, update CAQH profiles, and maintain active contracts. Without proper credentialing, reimbursement cannot begin.
Authorization Management
Prior authorization is often mandatory for therapy sessions. Delays can disrupt revenue cycles.
Denial Management
Experienced mental health billing specialist companies analyze denial patterns and correct root causes.
Medicare and Medicaid Billing
Billing Medicare for mental health services requires strict compliance with documentation standards and coverage limitations.
Telehealth Billing
With virtual therapy expanding nationwide, billing for mental health services must follow evolving telehealth policies.
Choosing the Best Mental Health Billing Services Company
Selecting the right partner requires more than comparing prices. Providers should evaluate:
Specialization
Does the company focus specifically on behavioral and mental health billing services?
Transparency
Are detailed monthly reports provided?
Technology Integration
Can the company work with your existing EHR system?
Experience
How long has the mental health billing company served practices in your state?
Support
Is there a dedicated account manager?
The best mental health billing services company does not just process claims. It acts as a revenue partner, proactively identifying financial improvement opportunities.
Cost Considerations and Value
Some practices search for a cheap outsource mental health billing company to reduce expenses. While affordability matters, extremely low rates may signal limited expertise.
Instead of focusing solely on cost, providers should measure:
-
Collection rate percentage
-
Days in accounts receivable
-
First-pass claim acceptance rate
-
Denial reduction trends
A top mental health billing company improves revenue enough to offset service fees.
Common Billing Errors in Mental Health Practices
Even experienced providers encounter billing mistakes. The most frequent include:
Incorrect time-based coding
Missing session documentation
Failure to verify eligibility
Improper use of telehealth modifiers
Expired credentialing
Billing for mental health therapists must align documentation with session duration and treatment plans. Inconsistent notes often trigger payer audits.
Outsourcing mental health billing reduces these risks by applying structured workflows and compliance reviews.
The Importance of Credentialing in Mental Health Billing
Many providers underestimate credentialing delays. Without active enrollment, billing for mental health services cannot proceed.
Mental health billing and credentialing services manage:
-
Initial payer applications
-
Revalidations
-
CAQH updates
-
NPI registration
-
Group enrollment
Timely credentialing ensures uninterrupted reimbursement and reduces patient billing confusion.
How Mental Health Billing Supports Practice Growth
Strong billing infrastructure directly supports expansion. When revenue is predictable, providers can:
-
Hire additional therapists
-
Expand telehealth programs
-
Open new clinic locations
-
Invest in patient experience
Billing services for mental health clinics create financial stability that supports long-term sustainability.
Practices partnering with the best mental health billing company often report higher collections and fewer compliance concerns.
Technology and Reporting in Modern Mental Health Billing
Today’s mental health billing solutions rely on analytics and automation. Detailed dashboards provide insight into:
-
Reimbursement trends
-
Payer performance
-
Outstanding claims
-
Patient balances
-
Revenue forecasting
Data transparency allows practice owners to make informed operational decisions.
Why Specialization Matters in Behavioral Health
Behavioral and mental health billing services differ significantly from other specialties. Mental health coding frequently involves psychotherapy add-on codes, crisis intervention billing, and evaluation and management combinations.
General medical billing for mental health without specialization may overlook these nuances. That is why many providers prefer mental health billing specialist companies with proven behavioral health experience.
Partnering With a Reliable Revenue Cycle Expert
As mental health practices navigate evolving insurance policies and regulatory updates, professional billing support becomes a strategic investment rather than an expense.
Organizations like 247 Medical Billing Services support healthcare providers through comprehensive medical billing services, medical coding services, and medical billing and coding services. Their expertise in revenue cycle management and credentialing services ensures smoother reimbursement processes for behavioral health practices seeking stability and growth.
Conclusion
Mental health billing services are more than administrative support. They are a critical foundation for financial health, regulatory compliance, and sustainable practice growth.
By partnering with an experienced mental health billing services company, providers can reduce denials, improve cash flow, and focus fully on delivering high-quality care to their patients. Whether you operate a solo therapy practice or a multi-location behavioral health clinic, investing in specialized billing expertise strengthens your long-term success.
Frequently Asked Questions
What are mental health billing services?
Mental health billing services handle claim submission, payment posting, denial management, and insurance follow-up specifically for therapy, psychiatry, and behavioral health practices.
Why is billing for mental health providers more complicated?
It involves time-based codes, strict documentation requirements, telehealth rules, and frequent payer-specific policy updates.
How does outsourcing mental health billing benefit small practices?
Outsourcing reduces administrative workload, improves reimbursement speed, and minimizes costly billing errors.
What should I look for in the best mental health billing services company?
Look for behavioral health specialization, transparent reporting, strong denial management processes, and credentialing support.
Can a mental health billing company help with Medicare billing?
Yes. Experienced providers manage billing Medicare for mental health services while ensuring compliance with federal documentation standards.
Is outsourced billing for mental health secure?
Reputable companies follow HIPAA regulations, use secure systems, and maintain strict data protection protocols.
How much does mental health billing typically cost?
Most companies charge a percentage of collections, often between 4 percent and 9 percent, depending on service scope and practice size.
Κατηγορίες
Διαβάζω περισσότερα
A Japan snowboarding trip offers one of the best winter sports experiences in the world. Every year, thousands of travelers visit Japan to enjoy deep powder snow, modern ski resorts, and beautiful winter landscapes. For travelers from Singapore, Japan is also one of the most convenient destinations for snowboarding adventures in Asia. Japan’s ski regions receive some of the heaviest...

Building a profitable online business requires smart sourcing and efficient distribution. Working with an Amazon wholesaler can be a game-changer for entrepreneurs looking to scale quickly. These wholesalers provide bulk products at competitive prices, allowing sellers to maintain healthy profit margins while meeting customer demand. One of the biggest advantages of partnering with a...

In today’s fast-moving digital world, music has become an ever-present companion. Whether you’re commuting, working out, studying, or just relaxing, having your favorite songs at your fingertips is essential. While streaming platforms like Spotify, YouTube Music, and Apple Music offer vast libraries, not everyone wants to depend on subscriptions or a constant internet connection....

Accessing your account smoothly is an important part of any online platform experience. While most users enjoy a seamless process, occasional login issues can happen due to technical or user-related reasons. If you are facing difficulties while accessing your account on Sky Exchange, there's no need to worry—most problems can be resolved quickly with a few simple steps. This guide...

In a globally interconnected food ingredients sector, Nutrich Foods Pvt. Ltd., headquartered in Kolhapur, Maharashtra, has emerged as one of India’s premier exporters of corn flaking grits—a crucial raw material for industries such as breakfast cereals, extruded snacks, and brewing. With a strategic vision, rigorous quality control, and a commitment to sustainability, Nutrich Foods...


