Community Behavioral Health Billing Massachusetts: Complete Guide for Providers in USA

Delivering community-based mental health services in Massachusetts is both impactful and complex. Providers operate within a highly regulated environment, balancing patient care with administrative demands. One of the most critical yet challenging areas is billing. From payer-specific rules to evolving compliance requirements, efficient billing can directly influence a provider’s financial health.
This blog provides a complete, practical guide to community behavioral health billing Massachusetts, helping providers streamline processes, reduce denials, and improve revenue outcomes.
Introduction
Community behavioral health services play a vital role in improving public health outcomes. However, billing for these services is not straightforward. Providers must navigate Medicaid, Medicare, commercial insurers, and state-specific guidelines.
Key points to understand:
- Billing accuracy ensures timely reimbursements and cash flow stability
- Compliance with Massachusetts regulations prevents audits and penalties
- Proper coding and documentation reduce claim denials
- Outsourcing can help providers focus more on patient care
Understanding Community Behavioral Health Billing
Community behavioral health billing involves submitting claims for services such as therapy, counseling, psychiatric evaluations, and case management. Unlike general medical billing, it requires a deeper understanding of behavioral health-specific codes, documentation standards, and payer rules.
A reliable community behavioral health billing agency ensures that claims are submitted accurately, reducing rework and delays. Providers often partner with a community behavioral health billing company to manage complex billing cycles and maintain compliance.
Why Massachusetts Requires Specialized Billing Expertise
Massachusetts has unique healthcare frameworks, including MassHealth programs and state-specific compliance mandates. This makes community behavioral health billing more complex compared to other states.
Key challenges include:
- Frequent policy updates and reimbursement changes
- Strict documentation requirements
- Integration with state-funded programs
- Coordination between multiple payers
Because of this, many providers seek a professional community behavioral health billing company to manage these complexities efficiently.
Core Components of an Effective Billing Process
A structured billing process ensures fewer errors and faster reimbursements. The essential components include:
Patient Eligibility Verification
Before services are provided, verifying insurance eligibility avoids unnecessary claim denials.
Accurate Coding
Using the correct CPT, ICD-10, and HCPCS codes is critical. Errors here can lead to claim rejection or underpayment.
Timely Claim Submission
Delays in submission can result in missed deadlines and revenue loss.
Denial Management
An efficient denial management system identifies root causes and prevents recurring issues.
Payment Posting and Reconciliation
Tracking payments ensures accuracy and highlights discrepancies.
A well-established community behavioral health billing services company typically handles all these aspects seamlessly.
Benefits of Outsourcing Community Behavioral Health Billing
Outsourcing has become a strategic choice for many providers in Massachusetts. It not only reduces administrative burden but also improves operational efficiency.
Improved Revenue Cycle Efficiency
Outsourcing community behavioral health billing services allows faster claim processing and reduced turnaround times.
Reduced Operational Costs
Instead of maintaining an in-house team, providers can benefit from cost-effective solutions similar to a cheap community behavioral health billing company Texas or other regions.
Enhanced Compliance
Experienced billing teams stay updated with changing regulations, ensuring compliance across all claims.
Focus on Patient Care
By delegating billing tasks, providers can concentrate more on delivering quality care.
Many organizations also explore outsourcing community behavioral health billing services Connecticut or outsourcing community behavioral health billing Virginia to compare efficiency and service quality benchmarks.
Key Features to Look for in a Billing Partner
Choosing the right billing partner is crucial. Here are the essential qualities to consider:
- Experience in community behavioral health billing
- Knowledge of Massachusetts-specific regulations
- Transparent reporting and analytics
- Strong denial management strategies
- Scalable services for growing practices
Top providers often compare options like a top community behavioral health billing company Texas or a top community behavioral health billing company Ohio to evaluate service standards.
Multi-State Billing Insights and Comparisons
While focusing on Massachusetts, it is helpful to understand how billing practices differ across states. For example:
- Community behavioral health billing services California often involve complex payer mixes
- Community behavioral health billing services Rhode Island may have stricter documentation checks
- Community behavioral health billing Maine focuses heavily on compliance audits
Similarly, providers may analyze services like community behavioral health billing services company Florida or community behavioral health billing services company Georgia to identify best practices.
Organizations operating across multiple states may also collaborate with a community behavioral health billing agency Delaware or a professional community behavioral health billing company New Hampshire for regional expertise.
Cost Considerations in Billing Services
Cost is a major factor when choosing a billing provider. While affordability matters, quality should not be compromised.
Options such as a cheap community behavioral health billing company South Carolina or a cheap community behavioral health billing company Virginia may seem attractive, but providers must ensure they meet compliance and performance standards.
Balancing cost and efficiency is key. The best community behavioral health billing company offers value through improved collections, reduced denials, and transparent pricing.
Technology and Automation in Billing
Modern billing solutions leverage advanced technology to improve accuracy and efficiency.
Electronic Health Records Integration
Seamless integration reduces manual data entry errors.
Automated Claim Scrubbing
Identifies errors before submission, reducing rejection rates.
Real-Time Analytics
Provides insights into revenue trends and performance.
AI-Driven Denial Prediction
Helps prevent claim denials before they occur.
Leading providers, including the best community behavioral health billing services company New York, utilize these technologies to optimize billing outcomes.
Common Challenges and How to Overcome Them
Despite advancements, providers still face several challenges:
Frequent Claim Denials
Solution: Implement strong pre-submission checks and coding accuracy.
Changing Regulations
Solution: Partner with a professional community behavioral health billing company Rhode Island or similar experts who stay updated.
Staff Training Issues
Solution: Continuous training and outsourcing specialized tasks.
Revenue Leakage
Solution: Regular audits and performance monitoring.
Providers comparing options like a best community behavioral health billing company North Carolina or best community behavioral health billing services company New Jersey often prioritize expertise in solving these challenges.
Why Choosing the Right Billing Company Matters
Selecting the right partner can significantly impact your practice’s success. A community behavioral health billing company California or community behavioral health billing company Georgia may offer insights into scalable operations and efficient workflows.
Ultimately, the goal is to partner with a best community behavioral health billing company that aligns with your practice’s needs and growth plans.
Conclusion
Community behavioral health billing Massachusetts requires precision, compliance, and expertise. As regulations evolve and payer requirements become more complex, providers must adopt efficient billing strategies to maintain financial stability.
Outsourcing to a reliable partner can simplify operations, reduce administrative burden, and improve revenue outcomes. Whether evaluating a community behavioral health billing services company or exploring multi-state providers, the focus should always be on quality, transparency, and long-term value.
For providers looking to streamline operations, integrating medical billing services, medical coding services, medical billing and coding services, revenue cycle management services, and credentialing services into a unified strategy can deliver significant improvements in efficiency and profitability. Organizations like 247 medical billing services help bridge operational gaps and ensure consistent financial performance.
FAQs
What is community behavioral health billing Massachusetts?
It refers to the process of managing and submitting claims for mental health services provided in community settings within Massachusetts, ensuring compliance with state and payer regulations.
Why is specialized billing important for behavioral health providers?
Behavioral health billing involves unique coding, documentation, and compliance requirements that differ from general medical billing, making specialized expertise essential.
Should I outsource my billing services?
Outsourcing can improve efficiency, reduce costs, and ensure compliance, especially for providers dealing with complex billing requirements.
How do I choose the best community behavioral health billing company?
Look for experience, transparency, compliance expertise, and strong denial management capabilities when selecting a billing partner.
What are the benefits of outsourcing billing services?
Benefits include improved cash flow, reduced administrative workload, enhanced compliance, and access to advanced billing technologies.
How can billing errors be minimized?
Using automated tools, accurate coding practices, and experienced billing professionals can significantly reduce errors and denials.
Catégories
Lire la suite
The Circulating Fluid Bed Boilers Market Size is witnessing steady growth as industries adopt advanced combustion technologies to improve energy efficiency and reduce emissions. As Per Market Research Future, circulating fluid bed (CFB) boilers are widely used in power generation and industrial processes due to their fuel flexibility, high combustion efficiency, and ability to handle low-grade...

In the world of streetwear, few moments create as much electricity as Black Friday. The day isn’t just about discounts — it’s about the chase. The thrill of scoring that rare hoodie or elusive piece from your favorite label fuels the same adrenaline that runs through sneaker drops and fashion collabs. And this year, Chrome Hearts and Comme des Garçons are at the top of...

The Specialty Chemicals Market continues to be a cornerstone of industrial innovation, enabling performance, differentiation, and sustainability across a broad spectrum of end‑use industries. Unlike commodity chemicals produced in bulk, specialty chemicals are formulated for specific functional properties — such as adhesion, corrosion protection, biocidal activity, rheology...

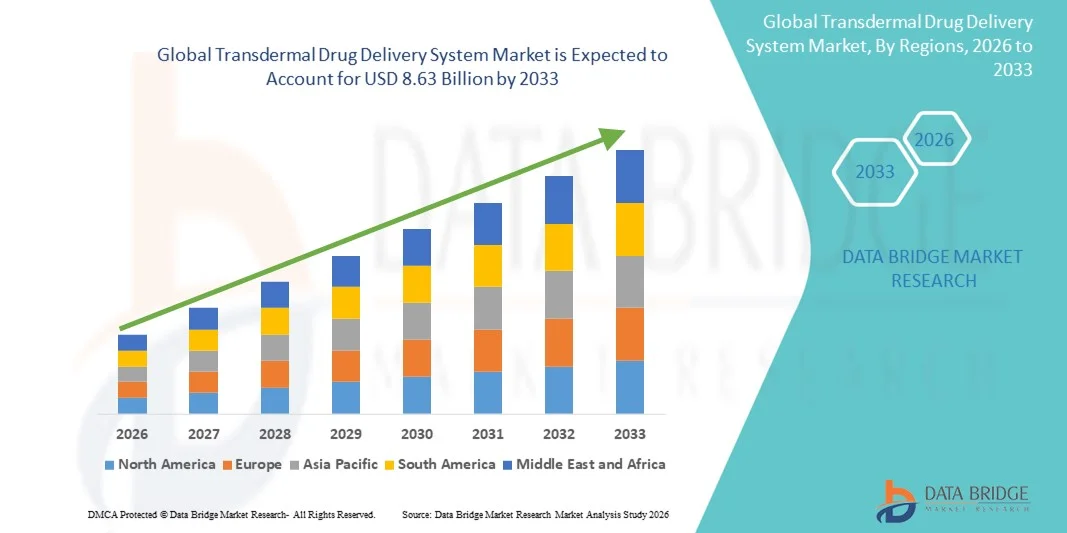
"Transdermal Drug Delivery System Market Summary: According to the latest report published by Data Bridge Market Research, the Transdermal Drug Delivery System Market The global transdermal drug delivery system market size was valued at USD 6.12 billion in 2025 and is expected to reach USD 8.63 billion by 2033, at a CAGR of 4.39% during the forecast...
Cracking open a digital pack in Pocket is still the closest thing to a jump-scare in a card game. One second you're half-asleep, the next you're leaning in like you can will an Immersive into existence. I started paying more attention to what I was actually chasing—art, EX lines, full sets—by browsing Pokemon TCG Pocket item cards first, then opening with a plan instead of pure...


